Low Salaries, Poor Facilities Deter Health Workers From COVID-19 Care

Mumbai, Delhi, Jaipur and Guwahati: Government and private hospitals are finding it difficult to recruit new and additional healthcare workers to care for COVID-19 patients even as the number of people testing positive continues to grow--1.59 million as of July 30, 2020--our reporting in five cities found.
The COVID-19 pandemic has added to the stress of an overburdened healthcare workforce. India has one medical doctor for every 1,404 people and 1.7 nurses per 1,000 people, according to the Ministry of Health and Family Welfare (MoHFW). This is lower than the World Health Organization (WHO) benchmark of one doctor and three nurses per 1,000 people.
During the early weeks of the outbreak in India in March and April, a combination of caution and fear pushed many healthcare professionals to return home. At the same time, small hospitals and healthcare facilities, which were shut for varying periods during the lockdown, cut down staff due to reduced revenues and uncertainty. This led to a shortage of personnel when they reopened.
As a result, nurses, ward boys, lab technicians, sanitation workers and other staff have been finding themselves stretched due to longer shifts and inadequate protection against COVID-19, medical and healthcare professionals told IndiaSpend in Mumbai, Hyderabad, Ahmedabad, Bengaluru and Kolkata. At the same time, fewer people are applying for vacancies for such jobs because of short-term contracts, low wages and poor working conditions, we heard from hospital staff, union representatives and city authorities.
State and private healthcare facilities that IndiaSpend reached out to have each sought to add at least a few hundred healthcare workers to ramp up care in COVID-19 wards since May.
“Not many people are applying for ancillary health positions possibly due to fears of COVID,” Abhishek Agarwal, a senior professor at Sawai Man Singh Hospital in Jaipur, Rajasthan, told IndiaSpend. “In some private hospitals, the number of staff has decreased, and doctors did not receive salaries for the lockdown months. In some other hospitals, doctors’ contracts have been changed from monthly salary basis to per patient basis.”
Low pay, short-term contracts
Hiring new health workers in the early days of the pandemic and the lockdown was difficult because of the fear of the infection spreading, said M.M. Prabhakar, superintendent of the state-run Ahmedabad Civil Hospital in Gujarat.
In West Bengal, more than 300 nurses quit their jobs in the early weeks of the COVID-19 outbreak to return to Manipur. To prevent a full-blown crisis, West Bengal chief minister Mamata Banerjee announced on May 18 that locals would be hired as helpers to replace nurses and trained to perform their basic functions in seven days.
In the same month, Ahmedabad was becoming a COVID-19 hotspot. The city's biggest COVID-19 facility, the Ahmedabad Civil Hospital, which has a daily requirement of 1,600 nurses according to hospital superintendent Prabhakar, had to rely on a pool of 125 nurses roped in from nearby hospitals and districts to complement their 1,308 nurses.
In June, the hospital attempted to recruit nurses on a three-month contract at a salary of Rs 13,400 per month, doctors and local nurses unions told IndiaSpend. The candidate turnout, they said, was low.
“This [Rs 13,400 per month] is not commensurate with the risk associated with [COVID-19] work,” said Vanraj Chauhan, general secretary of the All Gujarat Nursing Union (AGNU); the union has 7,000 members across the state from public and private hospitals.
The Ahmedabad Municipal Corporation (AMC) has since offered incentives along with salaries, and the Ahmedabad Civil Hospital has been able to hire staff to replace the healthcare workers who had been pooled from nearby districts, Prabhakar told IndiaSpend. The recruitment is still ongoing and salaries are in line with those specified by the state government, he said.
The southern states have been facing similar challenges. In June, the Telangana government sought to hire 509 healthcare workers, including 88 staff nurses, five pharmacists and 59 lab technicians, on contract for a year. The salaries on offer were Rs 23,000 per month for nurses, Rs 21,000 per month for pharmacists and Rs 17,000 per month for lab technicians, as per the state’s notification.
Starting salaries for non-contractual trained nurses in Hyderabad range between Rs 35,000 and Rs 40,000 per month, Shrikant Kalaskar, a Hyderabad-based public health professional, told IndiaSpend. “Government hospitals cannot expect staff nurses or doctors to work at a low salary in a metro city,” he said. “Raising the salary is a general requirement to hiring a professional, and this becomes more important during a pandemic.”
IndiaSpend reached out to J. Venkati, the district medical and health officer for Hyderabad, to understand the challenges in recruiting healthcare workers during the COVID-19 outbreak. This report will be updated as and when we receive a response.
In Karnataka’s capital, Bengaluru, the civic body, Bruhat Bengaluru Mahanagara Palike (BBMP), announced on July 21 that it would host walk-in interviews to hire doctors, nurses, health assistants and other medical staff--on a “purely temporary” basis--to manage COVID-19 patients in primary health centres. The BBMP hired 58 people in one day, N. Manjunatha Prasad, the BBMP Commissioner, noted in a tweet a day after the first walk-in interviews were held.
IndiaSpend reached out to Prasad and the BBMP to find out how many healthcare workers the city needs and the challenges in recruiting them. This report will be updated if and when they respond.

Recruitment announcements from the Bruhat Bengaluru Mahanagara Palike. A similar recruitment drive was conducted in Hyderabad.
Delayed salaries
Existing healthcare workers are unwilling to take on COVID-19 work due to poor working conditions in many public and private hospitals including long shifts and delayed and reduced salary payments, IndiaSpend found. This is despite guidelines issued in June by the Indian Council of Medical Research (ICMR) to prevent workers from being exposed to COVID-19 and the Supreme Court’s June 17 order on the timely payment of salaries.
There has been a reduction in salaries in several private hospitals across India. Healthcare staff in private hospitals in Kerala are facing a “forced loss of pay”, since the lockdown because private hospitals have restricted the number of days that staff work so that they are paid for fewer working days, said Roshan Radhakrishnan, a Kochi-based consultant anaesthesiologist. “This has been going on since March-April. We do not see an end to this.”
In April, the United Nurses Association (UNA), a national union representing 380,000 nurses, filed a petition with the Supreme Court seeking the government’s intervention to frame a policy for their welfare, including regarding non-payment of salaries, lack of personal protective equipment (PPE) in hospitals, long shifts and lack of access to adequate testing and quarantining. The court disposed of the petitions on April 15 after noting that the Central government had already established a helpline number for healthcare workers’ grievance redressal.
Later, in a judgement on a separate petition by Arushi Jain, a doctor, the Supreme Court on June 17 directed the central government to issue a notification so that health workers facing delayed salary payments could file a complaint against the hospital management under the Disaster Management Act, 2005 and under Section 188 of the Indian Penal Code, making the delayed payment of salaries a criminal offence.
“However, we still do not have established mechanisms for grievance redressal,” said UNA’s legal counsel Subhash Chandran K.R.
For instance, Chandran pointed out, the Hamdard Institute of Medical Sciences & Research (HIMSR) and its associated Hakeem Abdul Hameed Centenary Hospital (HAHC) in New Delhi had “abruptly fired 84 nurses on July 11 and that on the same day, it issued a walk-in interview notice to recruit nurses for a 12-month period at a lower pay scale”. The ousted nurses challenged their dismissal in the High Court of Delhi.
The nurses’ contracts had already expired and could not be renewed due to the lockdown, HAHC’s medical superintendent Sunil Kohli said in a letter to the Delhi government. Subsequently, Kohli said, 30 of the 84 nurses were given offers to extend their contracts after a reassessment.
“A lot of healthcare workers are jobless. The hospitals are using the pandemic as an opportunity to make more profits,” said Chandran, citing reports of hospitals overcharging for COVID-19 treatment. “But they are not paying their staff in time.”
The pandemic has also brought to the fore the differences in salaries and facilities that contracted healthcare workers and their peers employed on a permanent basis are entitled to. For instance, in Bihar’s capital, over 700 contract nurses at the All India Institute of Medical Sciences (AIIMS), Patna, struck work on July 23, bringing hospital operations to an absolute halt.
The strike came nearly a week after the contract workers sent a letter to the Institute’s director, Prabhat Kumar Singh, seeking provisions that are already available to the 120 regular nurses, including higher standard of care if they were to fall sick, increased remuneration and provision for leaves similar to that of permanent workers.
The central government, not the hospital director, is responsible for decisions regarding conversion to permanent status and salary hikes, Sanjeev Kumar, nodal officer for COVID-19 at AIIMS Patna, told IndiaSpend. The strike was called off after the hospital administration guaranteed that workers could avail free COVID-19 treatment at AIIMS Patna, increased the number of leaves for contract workers to eight days per month (four weekly offs and four leaves for doing night duties, which are carried out by all staff) and assured them that their contracts would be reviewed for the next one to two years barring disciplinary action, said Kumar.
Nurses will willingly work provided the government does not cut salaries, Prasanth Narayan, UNA general secretary in Karnataka, told IndiaSpend.
Lack of PPE usage guidelines
Healthcare workers across cities told IndiaSpend that they are bristling at the insensitivity regarding usage of PPEs and the absence of PPE guidelines.
The use of N95 respirator masks, which are a part of the PPE, should be avoided for longer than four hours, state the WHO guidelines on the rational use of PPE for coronavirus disease. The guideline does not specify any such usage limit for the complete protective suit.
The nursing staff often get dehydrated and suffer from low-blood pressure due to long and continuous wearing of PPEs, M. Rajeswari, a professor and president of the Telangana branch of the Trained Nurses Association of India (TNAI), told IndiaSpend.
“I work for 8-10 hours daily. We are given a replacement only if our PPE tears,” Akash Pillai, a nurse with Global Hospital, a private facility in Mumbai, and the general secretary of UNA Maharashtra, told IndiaSpend.
There is no shortage of PPEs in the hospital, an official from the branding and communications department of Global Hospital told IndiaSpend, on condition of anonymity. “We follow all protocols issued by the government but there is no standard guideline regarding the minimum time of usage for a complete PPE kit.” She refused to comment when IndiaSpend asked how many PPE suits one worker could use on a single shift.
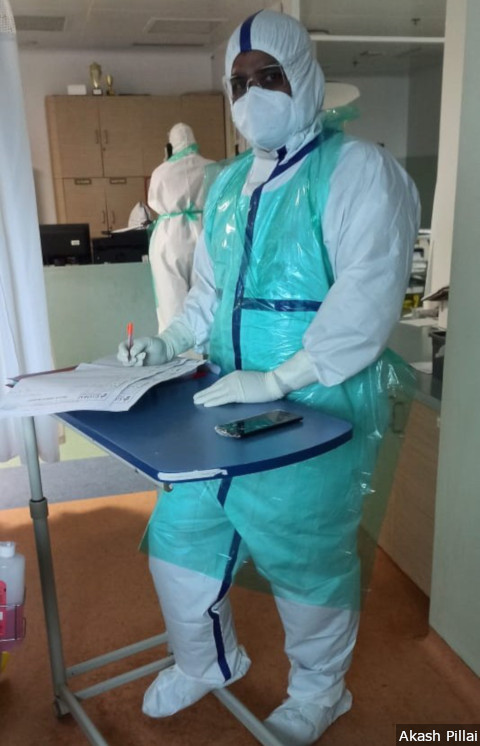
“I work for 8-10 hours daily. We are given a replacement only if our PPE tears,” says Akash Pillai, a nurse with Global Hospital, Mumbai, and the general secretary of UNA Maharashtra.
In West Bengal, the government capped the price that hospitals could charge patients for PPE in June. “Some private hospitals have since been limiting the availability of PPEs to health workers as they are unable to pass on the cost to the patients,” said Ranjith K. Raju, president of the UNA’s Kolkata chapter.
Quarantine measures are crucial to prevent transmission of the novel coronavirus SARS-CoV-2 from those believed to be exposed to it. Healthcare workers told IndiaSpend that they do not have space to isolate themselves as they live with their families. Across Karnataka, including in state capital Bengaluru, for instance, “there are no separate quarantine zones or accommodation facilities provided to nurses and doctors”, said Karnataka UNA’s Narayan. “This puts everyone at the hospital as well as their own families at risk.”
“Unless hospitals provide quality safety kits and implement quarantine protocols, health workers will not turn up for work even if they wish to,” said Kolkata UNA’s Raju.
Right incentives
Some states have managed to retain and recruit healthcare employees by offering incentives, increased salaries and boarding and lodging facilities.
In Maharashtra’s capital, Mumbai, the Brihanmumbai Municipal Corporation (BMC) calculated the bed-to-doctor and bed-to-nurse ratio to calculate the additional staff requirement, said Daksha Shah, the civic body’s deputy health officer. “We offered a strong remuneration package, ensured the availability of PPEs and guaranteed the safety of doctors and nurses. I think this strategy worked,” Shah told IndiaSpend. The BMC also recruited qualified ayurvedic and unani doctors for supervision purposes and hired nurses who were qualified and waiting for their degree, Shah said.
Shah was unable to state how many vacancies the civic body had filled, nor could she state the number of additional recruitments that have been made due to COVID-19. IndiaSpend also contacted Mangala Gomare, the BMC deputy executive health officer, but did not receive a response. This report will be updated if and when we receive a response.
One of the civic body’s recruits, Namrata Roy, explained how and why she ended up as a healthcare worker with the BMC. The 29-year-old has been working as a nurse at the Korba Mithaghar Municipal school, an isolation centre for asymptomatic patients in central Mumbai’s Wadala neighbourhood since May. She was employed a day after she sent an application to the BMC on May 21, and was asked to report for duty from the following day.
Roy is on a six-month contract with the BMC on a salary of Rs 50,000 per month. The civic body provides her free accommodation and food in a three-star hotel near the isolation facility, she said. “I am happy with the salary. I feel everyone is doing their best in this difficult time and so am I,” Roy told IndiaSpend on July 23, adding she is yet to receive her salary for the month of June. “I would have worked even if the salary was lower but as long as the government provided us with basic facilities and ensured our safety.”

Namrata Roy works as a nurse at a civic body-run centre for asymptomatic COVID-19 patients in Wadala, central Mumbai. She is on a six-month contract with the civic body, and receives free accommodation and food.
In Telangana, the state government provided a one-time incentive to employees of the health and medical departments, including to sanitation staff, under the Telangana Chief Minister’s Special Incentive plan in April. This has since been extended. “We received the 10% initiative,” said K. Vijayesh Kanth, a staff nurse at the Gandhi Hospital in Hyderabad. “This was a good boost for permanent employees but not so much for contract employees as their gross salary is low.”
Gujarat too relied on one-time incentives for doctors and nurses in government hospitals. “The AMC has brought in an incentive programme where doctors receive Rs 25,000 per month in addition to their salaries, and nurses and other medical staff get an additional Rs 15,000 per month,” Ahmedabad Civil Hospital’s superintendent Prabhakar told IndiaSpend.
When the Rajasthan state government faced difficulties in recruiting lab technicians to join the state’s COVID-19 labs in April, it chose to recruit them at more than double the pay grade under a different title. “The pay for technicians is Rs 7,000 but the government advertised for a research assistant position with a salary of Rs 18,000 and was then able to fill all vacancies,” said Sudhanshu Kakkar, the principal and controller of Rajasthan University of Health Sciences (RUHS), the dedicated COVID-19 facility in capital Jaipur.
In Jaipur, timely provision of on-demand testing for COVID-19, quarantine facilities, protective gear, and humane work conditions with fixed shifts and on-time salary ensured that the health workforce stayed motivated through the ongoing pandemic, as IndiaSpend reported on July 27.
Private hospitals can hire staff on longer contracts or recruit on a permanent basis to deal with the shortage of staff, say many healthcare professionals. Permanent hiring at increased salaries will also incentivise experienced professionals to apply for new positions, as opposed to the majority of current applicants who are fresh graduates with little-to-no experience, said AGNU’s general secretary Vanraj Chauhan, adding that Gujarat has 6,000-8,000 trained nurses that enter the workforce every year.
Longer contracts would also incentivise applicants. “Job security is important for everyone. Even if it is a contract position, it should be for a longer duration, say three or four years, to create a sense of security for the person,” said Hyderabad-based Kalaskar.
Those working in intensive care units should get special incentives as they work with the most critical patients, said Kakkar of RUHS.
Healthcare workers should also be provided with term life insurance and pay as per the Central Government Health Services (CGHS) scale, Giridhar Babu, professor and head of Life Course Epidemiology at the Public Health Foundation of India, told IndiaSpend. “They should be able to access dedicated beds, and new recruits should get incentives.”
“The pandemic is highlighting the importance of nurses worldwide,” and the WHO has declared 2020 the year of nurses and midwives, said Rajeshwari of TNAI Telangana. “If nurses are paid better, we will be better respected in society. Their status will rise, and there will be more people taking up nursing as a profession.”
(Jacob, a graduate from the National Institute of Criminology & Forensic Science, Bharadwaj, a recent graduate of Yale University, Saha, a graduate from the Symbiosis School of Economics and Inamdar, a graduate from Institute of Development Studies, are interns with IndiaSpend. Copy editing by Marisha Karwa. Shreya Khaitan contributed to this story.)
We welcome feedback. Please write to respond@indiaspend.org. We reserve the right to edit responses for language and grammar.


