Filthy Facilities Imperil Bihar’s Sterilised Women

Women at a healthcare facility which was part of a study on female sterilisation in Eastern Bihar.
- Women recovering from surgery lay on cotton mats on the floor.
- Many were discharged without being medically checked or told about post-surgery care.
- The floors of healthcare facilities were strewn with used syringes and bandages; walls were smeared with blood and windows—including those of operating rooms—were broken.
- With conditions ripe for infection, that is, in fact, what happened to more than half of all women in district hospitals.
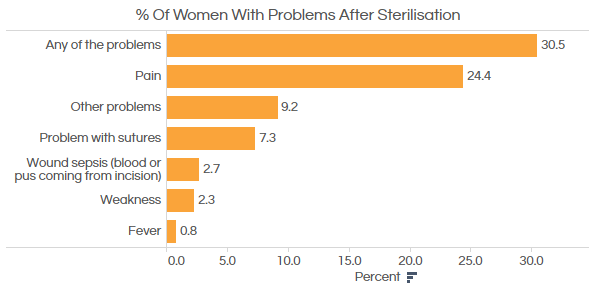 Source: ICRW The objective of the ICRW study was to provide evidence on the gaps in family planning services for women as well as efforts needed to improve the quality of such services in Bihar. These are some of the conclusions of the ICRW study:
Source: ICRW The objective of the ICRW study was to provide evidence on the gaps in family planning services for women as well as efforts needed to improve the quality of such services in Bihar. These are some of the conclusions of the ICRW study: - Health facilities lack private spaces to deliver family planning services, compromising the dignity of clients and the quality of services.
- Few facilities had enough drugs and equipment to effectively provide sterilisation and intrauterine contraceptive device services.
- Many health service providers and counsellors have limited interpersonal skills and professional training to deliver quality family planning services to women.
- Unsanitary conditions at most facilities demonstrate disregard for infection prevention
- Women want cleaner facilities with better interaction with and care from providers.
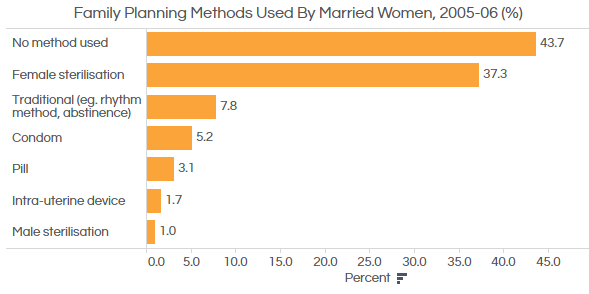 Source: National Family Health Survey High risk of simple sterilisation In an incident that led to much soul-searching in India last year, 16 women lost their lives in Chhattisgarh to failed sterilisation procedures. This was not an aberration, as IndiaSpend reported. Our analysis of national health data revealed 200 deaths ever year between 2009 and 2011. A preliminary inquiry into the Chattisgarh deaths revealed that the first camp held on November 8, 2014, carried out 137 operations, ignoring government orders restricting sterilisation operations per day to 30, India’s Minister for Health and Family Welfare, Jagat Prakash Nadda said in a statement to the Lok Sabha. Nadda also said the operation theatre was not working, and adulterated medicine was given to the women who died. However, larger questions emerged after the incidents regarding better practices at health centres. The ICRW report from Bihar indicates that while there have been some improvements over the years in physical infrastructure, such as electricity and water, other problems were widespread and severe. __________________________________________________________________ “Liked this story? Indiaspend.com is a non-profit, and we depend on readers like you to drive our public-interest journalism efforts. Donate Rs 500; Rs 1,000, Rs 2,000.”
Source: National Family Health Survey High risk of simple sterilisation In an incident that led to much soul-searching in India last year, 16 women lost their lives in Chhattisgarh to failed sterilisation procedures. This was not an aberration, as IndiaSpend reported. Our analysis of national health data revealed 200 deaths ever year between 2009 and 2011. A preliminary inquiry into the Chattisgarh deaths revealed that the first camp held on November 8, 2014, carried out 137 operations, ignoring government orders restricting sterilisation operations per day to 30, India’s Minister for Health and Family Welfare, Jagat Prakash Nadda said in a statement to the Lok Sabha. Nadda also said the operation theatre was not working, and adulterated medicine was given to the women who died. However, larger questions emerged after the incidents regarding better practices at health centres. The ICRW report from Bihar indicates that while there have been some improvements over the years in physical infrastructure, such as electricity and water, other problems were widespread and severe. __________________________________________________________________ “Liked this story? Indiaspend.com is a non-profit, and we depend on readers like you to drive our public-interest journalism efforts. Donate Rs 500; Rs 1,000, Rs 2,000.” Next Story


